Ignorance… What Almost Cost Me And/Or My Baby’s Lives
March 19, 2026 By Kaylee Campbell
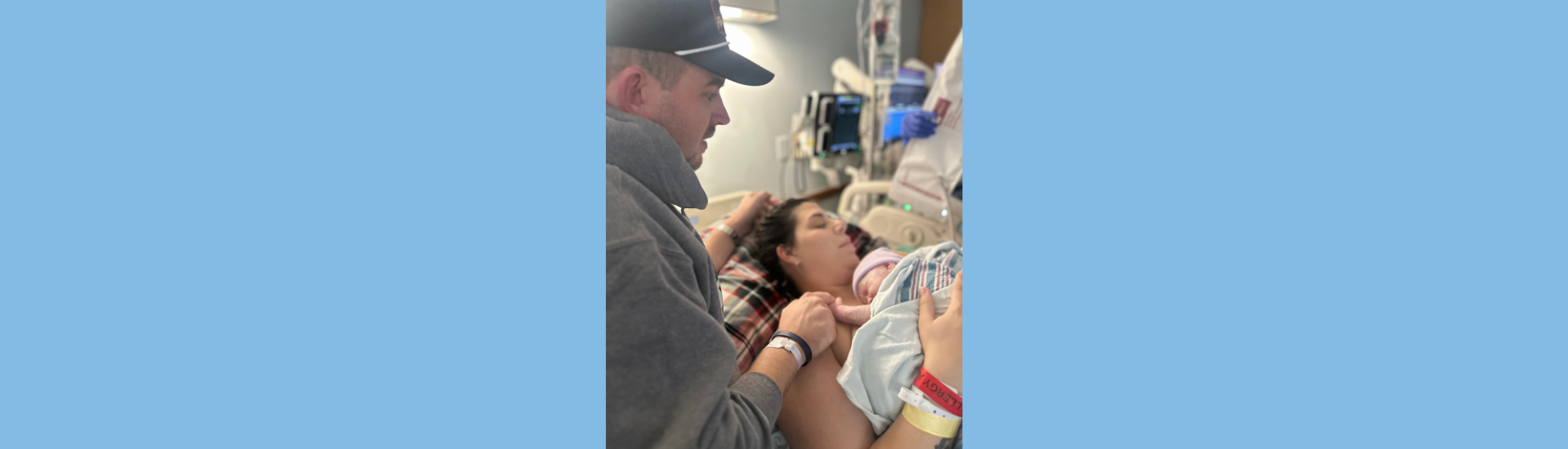
My name is Kaylee. After a year of infertility, my husband and I were overjoyed to be expecting our baby girl in December 2025.
At 35 weeks pregnant, I began having daily headaches that would not go away. Around the same time, I noticed my blood pressure creeping into the 130–140s systolic range, which was higher than it had been throughout my pregnancy. I contacted my midwife to share my concerns and was told by her medical assistant to stop checking my blood pressure at home and come in for a visit.
At my appointment, my midwife repeated the same advice, saying checking my blood pressure was causing unnecessary worry. I am a registered nurse and know my body well, so I was concerned, but I followed their recommendation.
At my 36-week appointment, I had gained 6 pounds in one week and had significant swelling in my hands and feet. My blood pressure was in the 140s, but again I was told everything looked fine. No labs or urine testing were done.
After that visit, I started checking my blood pressure again at home. It continued creeping into the 140–150/90 range.
At my 37-week appointment, I presented with the same symptoms I had been having for over two weeks. My blood pressure was 142/86, and this time my midwife sent me directly to labor and delivery triage.
At the hospital, they ran labs, a urine analysis, and placed me on monitors. I had a severe headache that did not improve despite medications and IV fluids. My urine tested positive for protein and I was also having consistent contractions. My repeat blood pressure was 148/91. With my labs, blood pressure, and persistent headache, I was diagnosed with preeclampsia with severe features. I was started on a magnesium drip to prevent seizures and told I needed to be induced immediately.
Due to a generator failure, I had to be transferred by ambulance to the main campus hospital. By the time I arrived, my blood pressure had climbed to 167/94 and I felt extremely unwell.
Overnight I required multiple blood pressure medications and Pitocin for induction. At 12:08 pm the next day, I delivered my beautiful 6 pound 13 ounce baby girl.
After delivery, I experienced a severe postpartum hemorrhage and required several medications and aggressive clot removal. I remained on magnesium for 24 hours postpartum and needed IV medications for extremely high blood pressures. I was discharged two days later but remained on two blood pressure medications for 12 weeks postpartum.
My placenta pathology later showed multiple blood clots caused by hypertension, which could have led to placental insufficiency, growth restriction, fetal stroke, or stillbirth. There were also findings of malperfusion due to hypertension.
Reading that was both terrifying and frustrating, knowing how often my concerns had been brushed aside. When I shared my frustration, my midwife told me, “Sometimes we, as practitioners, ignore our patients’ concerns. We need to take everyone more seriously.”
I’m sharing my story to encourage pregnant women to advocate for themselves and their babies. Trust your instincts and speak up until you are heard. I’m incredibly grateful that my daughter and I are healthy, but I can’t help but wonder how many others have been dismissed and had far worse outcomes.

In 2024, my husband and I received our long-awaited answered prayer—the pregnancy and birth of our first child, our daughter, Shira. Wh...
ReadMore- It Just Started With A Headache May 06, 2026
- Know the Signs and Take Action May 06, 2026
- My Preeclampsia Journey: Three Pregnancies, Three Different Paths May 06, 2026
- Eager May 06, 2026
- “you’re Fine.” Until You’re Not. May 06, 2026
- Casey & Charlie’s Story May 06, 2026
- Pre and Postpartum Preeclampsia May 06, 2026
- I had never heard of preeclampsia May 06, 2026
- 2x Survivor Of Preeclampsia May 06, 2026
- My Preeclampsia Story May 06, 2026
